Introduction
A person’s heart does not operate on a schedule. It cannot be observed beforehand or wait to be observed. Many cardiac episodes occur outside the clinical setting, during normal daily activities. An ECG in the clinic may appear normal at a brief moment, while symptoms continue. This is where the Holter monitor fits in. It allows continuous recording of heart activity and provides the opportunity to observe the condition in daily life.
Origin and Development
The Holter monitor was developed in the 1940s by Norman J. Holter with the aim of recording the heart’s electrical activity outside the laboratory. Early devices were large and difficult to manage. They required substantial supporting equipment and were not practical for regular use. With advances in technology, smaller and portable versions were developed. This made continuous ambulatory monitoring possible and changed how cardiac rhythm is evaluated.
The Device
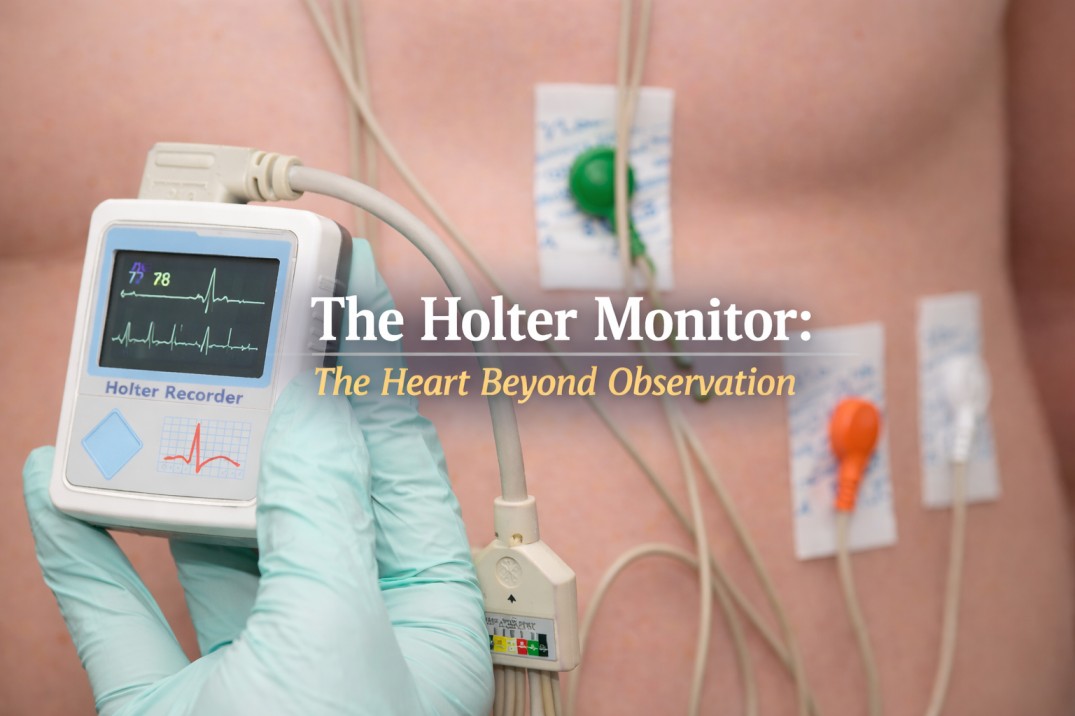
A Holter monitor is a portable device that records the electrical activity of the heart. Patients typically wear it for 24–48 hours or longer while performing their everyday activities. During this time, it records continuous cardiac activity. The device consists of electrodes applied to the chest and a small recording unit that allows mobility. It captures heart rate, rhythm, and electrical patterns over time. Unlike a standard ECG, which provides a single snapshot, the Holter monitor records continuously.
The Role It Plays
The Holter monitor is used to assess intermittent cardiac abnormalities that may not be detected on a routine ECG. It helps identify arrhythmias, pauses, and transient rhythm changes. It also allows correlation between patient symptoms and cardiac activity. Symptoms such as palpitations or lightheadedness can be documented and compared with the recorded data. This provides a clearer picture of the patient’s condition in real-world settings.
What Makes It Critical
The heart’s rhythm is dynamic and changes throughout the day. Abnormalities can occur suddenly and without warning. A Holter monitor records these changes over an extended period, providing a more complete picture of cardiac rhythm. Even brief episodes can have clinical significance. Continuous monitoring captures data that cannot be obtained from a single, short recording.
Where Errors Begin Quietly
Small errors can occur during Holter monitoring. Poor electrode placement may reduce signal quality, while loose leads can interrupt recording. Patient activity also affects results. Reduced activity or changes in routine may limit the occurrence of symptoms during monitoring. Incomplete symptom documentation can make interpretation more difficult. The Holter monitor will still produce data, but the quality may be affected.
The Illusion of Completeness
Continuous monitoring can create the impression of a complete picture, suggesting that all relevant cardiac events will be captured. However, it is limited to the monitoring period. Events occurring outside this timeframe will not be recorded. Interpretation also depends on signal quality and clinical context. While the recording is continuous, it does not provide complete understanding of all events.
Why It Matters
Accurate detection of cardiac abnormalities is essential for effective patient management. Missed arrhythmias can delay diagnosis and treatment. By providing extended monitoring, the Holter monitor supports clinical decision-making and helps guide further evaluation and therapy. It can also help avoid unnecessary procedures when findings are clear. This makes it a valuable tool in clinical practice.
Closing Thought
A Holter monitor allows extended evaluation of the heart beyond the clinic and captures how it functions in daily life. However, it does not remove uncertainty. It records the heart’s rhythm, but the results require interpretation. That interpretation determines whether a cardiac problem is present.